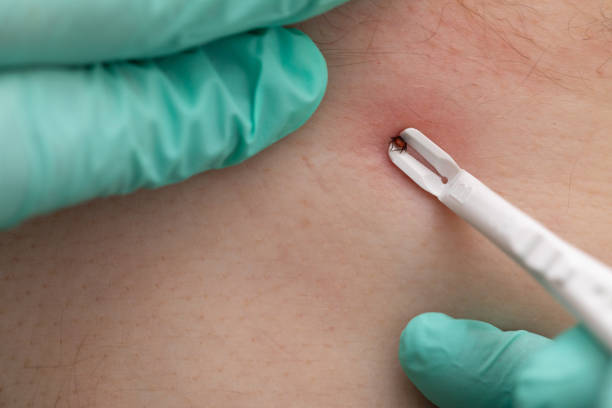
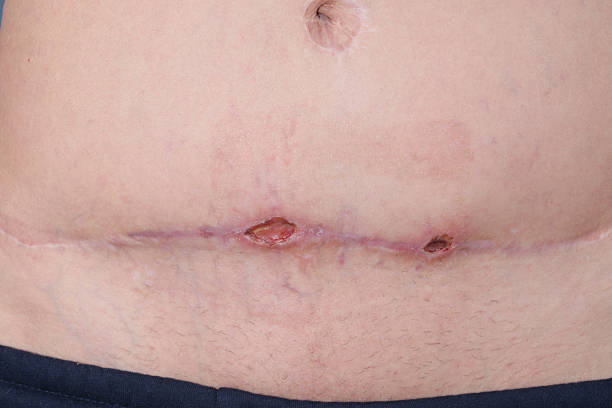
NON-ALCOHOLIC FATTY LIVER DISEASE
September 16, 2022
HASHIMOTO’S THYROIDITIS
September 19, 2022Vitiligo is a chronic (long-lasting) skin pigmentation disorder that causes white or lighter patches of skin to appear on various parts of the body. Vitiligo impacts people of all skin types, races and genders. It is estimated that 1% of the global population has vitiligo.
It is not life-threatening or contagious but has no cure. Meanwhile, treatment may help in making the skin tone appear more even.
The cause of vitiligo is unknown. Meanwhile, there are speculations that it could be a result of certain autoimmune disorders, genetic factors, neurologic factors and the self-destruction of melanocytes. Melanocytes are cells that produce the pigment of the skin. When attacked or destroyed either by the immune system or due to self-destruction, the pigmentation of the skin is affected.
The types of Vitiligo are Generalized Vitiligo, Segmental Vitiligo, Mucosal Vitiligo, Trichrome Vitiligo, Universal Vitiligo and Focal Vitiligo.
The risk factors for Vitiligo are family history of vitiligo, family history of autoimmune disorders (like Addison’s disease, rheumatoid arthritis, thyroiditis, psoriasis, Type 1 diabetes, systemic lupus erythematosus and pernicious anaemia), previous skin issues and trigger events (like stress, sunburn and skin trauma).
Symptoms of vitiligo are loss of natural colour or pigment of the skin, hair and mucous membranes, inflammation of the eye, inflammation of the ear and low self-esteem.
The complications of vitiligo are problems with impaired hearing sunburn and psychological distress.
Laboratory diagnosis of vitiligo is by Antinuclear Antibody Screening, Complete Blood Count and Skin Biopsy.
Certain medications, repigmentation therapy, light therapy, surgery and counselling can be used in the treatment of vitiligo.
Visit MedBioTech for a complete blood count, skin biopsy and antibody screening for an accurate diagnosis of vitiligo.
References:
my.clevelandclinic.org
www.mayoclinic.org
www.niams.nih.gov