PERTUSSIS (WHOOPING COUGH)
March 5, 2023
AUTOIMMUNE PANCREATITIS
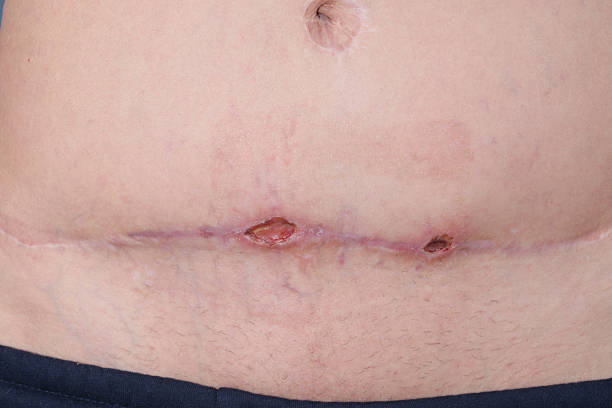
March 12, 2023Any surgery that results in a break in the skin can cause an infection, despite the numerous safeguards and protocols in place to prevent infection. These infections are known as Surgical Site Infections. They are the most frequent type of healthcare-associated infection (HAI) observed on admission in low- and middle-income countries (LMICs).
These infections are known as Surgical Site Infections (SSIs) by doctors because they develop on the area of the body where the surgery was performed. If a person undergoes surgery, the chances of developing SSI are about 1% to 3%.
Types of Surgical Site Infections (SSI) are Superficial Incisional SSI, Deep Incisional SSI and Organ/ Space SSI. SSI occurs within 30 days after surgery.
Surgical Site Infections are caused by germs at the site of surgery. Some of the organisms most commonly isolated in SSI are Staphylococcus, Streptococcus and Pseudomonads species.
The risk factors of SSI are having other diseases, surgeries that last more than 2 hours, being elderly, smoking, being overweight, having cancer, emergency surgery and abdominal surgery.
Symptoms of SSI are fever, chills, sweats, cough, bad smell from the site of surgery, sore throat, pain, pus at the site of surgery, redness, delayed healing, swelling and abscess.
The complications are delayed and non-healing of the wound, cellulitis, abscess formation, osteomyelitis and further wound breakdown.
The laboratory diagnosis of Surgical Site Infection is through laboratory tests such as full blood count, wound swab microscopy and culture, erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP).
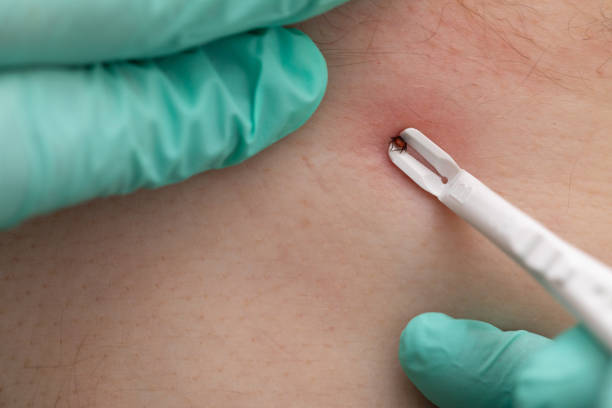
SSI can be treated with additional surgery, consistent antibiotic therapy, wound drainage, and rigorous wound debridement.
To prevent Surgical Site Infection, avoid smoking, maintain a healthy weight, avoid touching wounds and ensure proper hand washing by visitors and caregivers.
Visit MedBioTech for reliable laboratory tests.
References:
www.cdc.gov
www.hopkinsmedicine.org
www.pubmed.ncbi.nlm.nih.gov